News

Life Expectancy Rose Slightly In 2018, As Drug Overdose Deaths Fell
< < Back toFor the first time since 2014, death rates in the U.S. declined and life expectancy showed a modest uptick, according to new data released in two reports Thursday by the Centers for Disease Control and Prevention.
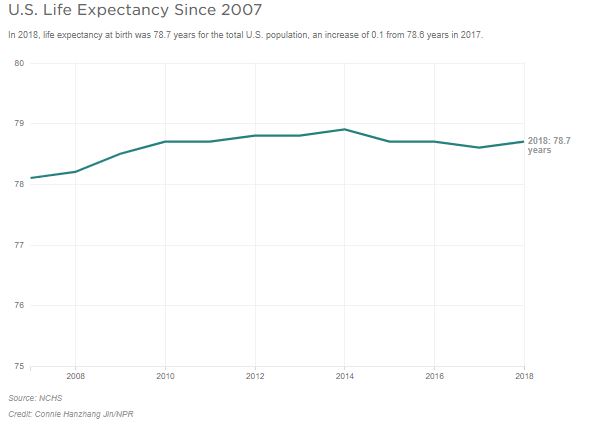
Life expectancy at birth in 2018 was 78.7 years, 0.1 year longer than the previous year.
It may seem like a small increase, but for a population of around 350 million, the shift represents improvements in the lives of many people, says the CDC’s Bob Anderson, the chief of the Mortality Statistics Branch at the CDC’s National Center for Health Statistics, who oversaw the new reports.
“That’s a lot of people who … avoided premature death,” he says.
The average lifespan of an American had risen for decades, reaching 78.9 years in 2014. But it took a dip in 2015, held steady in 2016 and dipped again in 2017, largely driven by the steep growth in drug overdose and suicide deaths.
Don’t see the graphic above? Click here.
The recent improvement was driven by decreases in death rates from six of the 10 leading causes of death, including a 2.2% decrease in cancer deaths (part of an ongoing downward trend since the 1990s) and a 2.8% fall in deaths from unintentional injuries, which include drug overdoses.
The new numbers show that in 2018, there were 4.1% fewer drug overdose deaths than in 2017, mostly in deaths involving natural and semi-synthetic opioids. That “includes drugs like oxycodone, which are commonly available by prescription,” says Anderson. “We [also] saw declines in deaths involving methadone and even … heroin.”
This is good news, says Dr. Daniel Ciccarone, a professor of medicine and an addiction researcher at the University of California, San Francisco. “It’s really the first positive change that we’ve seen in a 20-year-long trend of drug overdose deaths.”
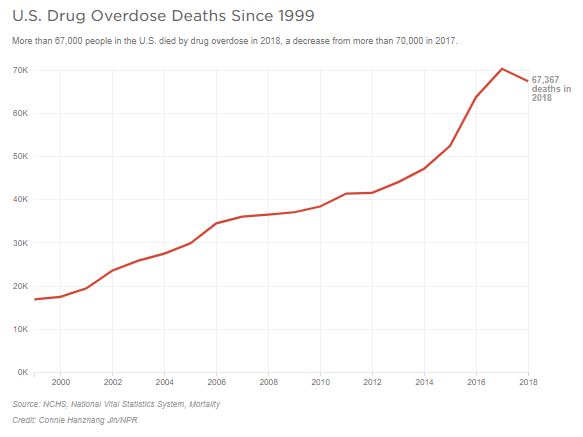
As the new report shows, drug overdose deaths had risen every year since 1999, until 2018.
Don’t see the graphic above? Click here.
“I think these numbers suggest that some positive news is starting to come out of the many efforts to try to stem the tide on overdoses,” says Kathryn McHugh, a psychologist at McLean Psychiatric Hospital and Harvard University.
Those efforts include improving access to treatment for opioid use disorder and access to overdose rescue, she notes.
But the new data “need to be interpreted with the utmost caution,” she says. “I don’t think we can interpret this as a win based on one year.”
After all, more than 67,000 people still died from drug overdoses in 2018, says McHugh. That’s “still a tremendously high number of fatalities.”
Besides, she adds, the decrease in deaths from opioids wasn’t uniform around the country. Fourteen states and the District of Columbia showed a decrease, whereas five states — California, Delaware, Missouri, New Jersey and South Carolina — saw an increase, and the other states didn’t change significantly.
“This has been an issue that has varied regionally from the very beginning,” says McHugh.
Also, the improvement in drug overdose deaths “could be a one-year pause in a continuing trend,” says Ciccarone.
Troubling new addiction trends emerge
He also points to more sobering data in the new report — the continuing increase in deaths from other drugs, especially synthetic opioids like fentanyl, but also stimulants like cocaine and methamphetamine.
The rate of deaths involving synthetic opioids (except methadone) increased by 10% between 2017 and 2018, according to the new report. The rate of overdose deaths involving cocaine increased by an average of 27% per year from 2012 to 2018. The rate of deaths involving stimulants like methamphetamine also increased on average by 30% annually during that time period.
“It’s worth noting that in many instances those stimulants are combined with opioids,” notes Anderson. “So it’s fairly common to see fentanyl and methamphetamine, for example, or fentanyl and cocaine mixed together.”
The use of a combination of drugs has increased over time, he says. “We seem to have sort of traded one set of drugs for another.”
Ciccarone calls this disturbing trend the “fourth wave of the opioid crisis,” following a first wave fueled by prescription pills, a second wave from heroin and third, starting in 2014 from synthetics like fentanyl.
The drug combinations makes addiction a harder problem to tackle, he says. “The crisis deepens because of the poly-drug phenomenon.”
McHugh agrees. “If we ignore that part of the crisis, we are going to see these numbers probably move in a bad direction,” she says.
Tackling this will need a serious look at prevention efforts.
“We have to move away from this understanding that we’re just going to treat it as a supply-side phenomena,” Ciccarone says. “As ‘let’s stop the opioid pills, let’s stop the excess prescribing.’ ”
Instead, we also have to address what’s driving the demand for these drugs in communities, he says.
“There’s a large amount of social, economic, spiritual despair in this country,” says Ciccarone. “And because we’ve underappreciated that phenomena, we’ve under-appreciated that there’s a demand side to problematic drug consumption.”
Addressing that despair, he says, will be key to preventing more people from turning to drugs in the first place.
Suicide rates still rise, but slower
Among other leading causes of death, the new data also showed a 1.4% rise in suicide deaths rates between 2017 to 2018. “It’s sadly consistent with previous years,” says Jerry Reed, a suicide prevention expert and the senior vice president for practice leadership at Education Development Center, a non-proft organization. “We’ve seen a gradual incline in suicide deaths from about 2000 until the present.”
But he also sees a glimmer of hope in the new numbers — the rate of increase of suicide deaths had slowed down. It was “markedly lower than the 4.4 % increase we saw from 2016 to 2017,” he says.
He says the change likely reflects the cumulative effects of years of suicide prevention efforts. That includes having a national strategy for suicide prevention, a national suicide hotline for people in suicidal crisis, training health workers in hospitals and clinics in suicide prevention, and funding for prevention efforts and mental health care access for youth.
“We [now] have an awareness in our nation that suicides are preventable, not inevitable public health problem,” says Reed. “And I think we’re beginning to see the fruits of our labor. Now, it’s that that moment when we need to keep the light on and keep the investments coming so that people who struggle don’t have to do so in silence.”
Overall, the new CDC data suggest that “we certainly can’t take our foot off the gas,” says McHugh. “If anything, we should be pushing harder on the public health [front] and try to continue to make progress.”
9(MDI4ODU1ODA1MDE0ODA3MTMyMDY2MTJiNQ000))